The Future of Insurance Claim in the Era of Technology Disruption
Innovation in technology plays a vital role in every aspect of the insurance business, especially changing the business models of insurers with an impact on every activity- both internal (actuarial, underwriting, etc.) and external (sales, marketing, distribution, customer service, etc.)
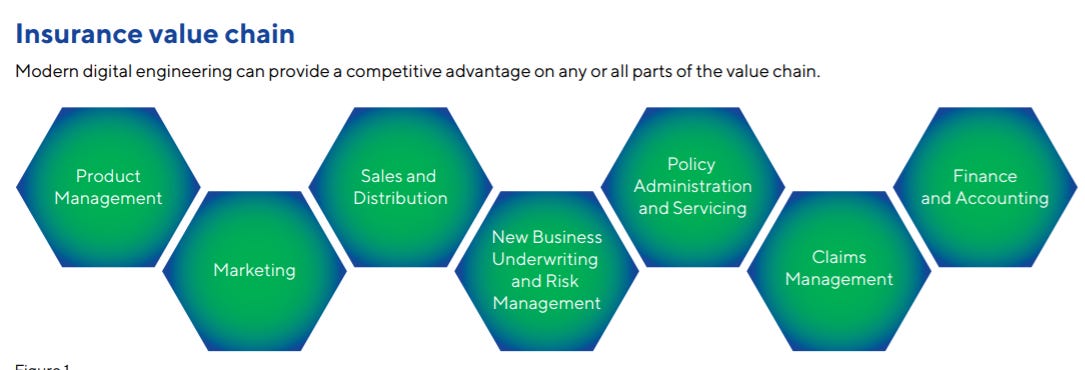
Primarily, the insurance sector was dependent on legacy systems like human interaction, human call centers, paper-based verifications, manual underwriting, and fixed pricing. However, after embracing new technologies, they are gradually improving operations in every area of the insurance value chain.
Source: Accenture
The activities that build up the insurance value chain, as well as technology innovations, can be visualized with the tools integrated to create a new form of communication, exchange of information, and customer relations. Automation makes it easy for insurers to run their operations smoothly and consistently.
The automation integration helps both insurance companies and claimants to coordinate effectively. Technology makes operations easy and helps clients or customers achieve desire outcomes fast. Technologies including AI, robotics, IoT, Blockchains, machine learning, API integration, etc. play a major role here.
The insurance company heavily depends on data points. In such scenarios, the rise of big data acts as a disruptive force. For example, predictive analytics integrated with big data can accurately compute pricing and risk selection, lower the underwriting costs and improve claims and develop with emerging trends.
Stats: A 2018 study from Valen Analytics found that companies that used analytics and predictive modeling saw their loss ratios improve 3% – 9% more than companies that didn’t. They also reported that insurers using predictive analytics grew their direct written premiums by 53%, compared to the market average of 18% growth during the same time period.
Artificial Intelligence and Machine Learning increase the automation processes in claim processing and employee insurance sectors. They help in fraud detection, surveillance, and preventions, claim process, and overall process efficiency.
Stats: A Deloitte Digital report stated that, as of 2017, more than 35.6 million people in the U.S. alone have voice-activated AI assistants, and the worldwide spend on these technologies was expected to reach $47 billion in 2020.
An SMA survey found that 66% of P&C insurance executives believe that machine learning has a high impact potential for commercial lines of business, while 53% of executives believe it has a high impact potential for personal lines.
The combination of IoT and IoT technologies allows real-time monitoring that has been useful for auto, P&C, and even health insurers. It aids in lowering the claims by making data accessible more accurately and in real-time, hence improving the efficiency of the entire insurance process.
Stats: P&C insurers can’t afford to delay in leveraging IoT capabilities, as forecasts project a global IoT insurance market value of $42.76 billion by 2022.
According to a McKinsey report, “30 or fewer manual processes account for 40% of an insurer's cost of doing business and 80% of customer activity. In digitizing or automating these processes, firms can eliminate up to 25% of manual labor costs. Automation is now essential across all functions of the value chain.”
Digital innovation and disruptive technologies are likely to enhance the future of insurtech. By leveraging the latest insurance technologies to reduce costs for both customers and insurers not only improves operational efficiency but also enhances the entire customer experience.
A fully integrated enterprise insurance software, ALFRED, provides the ability to leverage smart automation like AI and Data in building a 360 ecosystem to transform how real-time claims processes can be settled.
The benefits include:
Automated documents digitization [printed, scanned, handwritten] > 90% Accurate
Fraud & abuse detection >30%
Reducing TAT up to 90%
Real-time claims status update, share documents, etc. without sending over email/WhatsApp, etc.
Self-learning and evolving system for better risk assessment, fraud, and decisions making.
Easy customized to the need for users to connect to any core claims system or use independently.
Digital Tarif/SOC management system for approval, update and use [without investing time for hospital manual contracts, record, and negotiation]
Real-time decision-making engine for providers and payers via Auto-adjudication and claims denial solutions.
To know more or interested in our product please CLICK HERE for the DEMO. Interested to know more, write to contact@artivatic.ai, and Artivatic will get in touch with you.